The Truth About Colonoscopy: Be informed before giving consent (Part 1)
A Short History of Colonoscopes
The first fiberoptic colonoscope was developed by Drs. William Wolff and Hiromi Shinya of Beth Israel Medical Center in New York City in 1969. This was a huge leap forward over a rigid pipe, called a sigmoidoscope, previously used to peer into the rectum of patients who had signs of cancer. The flexible scope allows the practitioner to examine the entire length of the colon. By 1973, more than 5,000 colonoscopies had been performed, demonstrating the utility and relative safety of the procedure.In 1983, the Welch Allyn Corporation invented the first video endoscope, allowing doctors to see the procedure and view the colonic mucosa on-screen. Previously, they could only see the tissues through a small eyepiece.
Although the exam was continually recommended from its inception, it wasn’t widely embraced until the American Society of Gastroenterology published screening guidelines in the early 2000s. Since then, the recommendations have been updated several times, with the most recent guidelines recommending a baseline screening at 45 years of age (previously, it was 55yo) and the timing of a follow-up screening based on the results/finding of the baseline exam. (R)
More than 15 million colonoscopies are performed each year in the U.S. The median cost of a colonoscopy in the US is $2,750; prices can range from $1,250 to $4,800 and more. The fees vary across different regions and can vary greatly if the screening is done as an outpatient vs inpatient procedure. Doing the math – 15M scopes x $2750 each– you’ll find that colonoscopies are a $41.25Billion/yr industry.
More Costs To Consider
- Uninsured patients will likely be responsible for the total cost of their exam.
- Patients with health insurance will be responsible for paying their deductible, copay, and coinsurance amounts. The amount will depend individual health plans.
- Other expenses may include: the cost of the prep, cost of pain medications after the procedure,and of course, if there are complications, fees and costs may soar.
This site, called New Choice Health, allows you to search for the best pricing in your area.
With so many people out of work, under-employed, or without medical insurance coverage, be sure to shop around for the best pricing on any medical procedure you may be having, not just a colonoscopy. You may be very surprised what you may find by reviewing this site.
What Does a Colonoscopy Procedure Entail?
Prior to the exam, you must clean out your colon so the physician has a clear visual field for examining the lining of your colon. This site gives a good overview of what to eat and how to best prep your colon before your procedure.
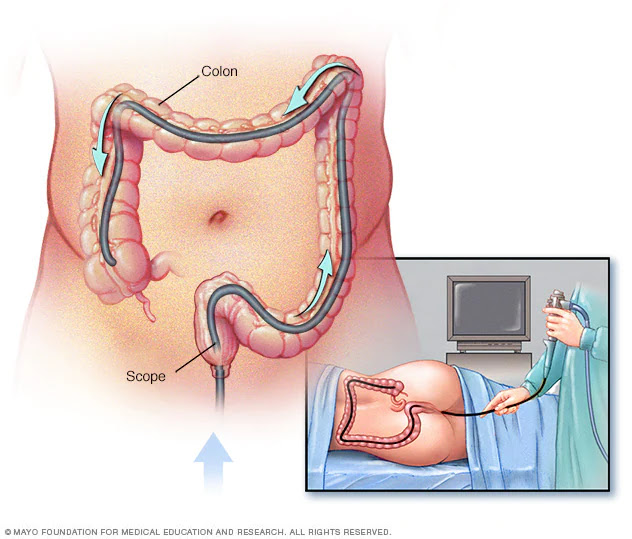
During the procedure, a long, flexible tube (colonoscope) with a tiny video camera is inserted into the rectum. Scopes can vary somewhat in size but most commonly, they are 168cm (66 inches) long and about 13mm (0.5 inches) in diameter. The time required to complete the scope can vary greatly, from less than 10 minutes to more than 60 minutes in difficult cases.
Conditions that can prolong the procedure include inadequate bowel cleansing (most common), advanced age, constipation, surgical history, and low body mass index (BMI). If necessary, polyps or other types of abnormal tissue can be removed through the scope during a colonoscopy.
A Word About Polyps
Polyps are irregular growths in your bowel. They are classified based on size and type to determine their risk of becoming colorectal cancer. While colon cancer is found in only about 40 out of 10,000 screening colonoscopies, almost all screens result in removing a polyp. In a study of 906 patients, aged 40 to 49 who had colonoscopy screening, it was found that at least 250 persons, maybe up to 1000 persons or more would need screening to detect one cancer. In financial terms, that would mean between $687,000 and $2,750,000 would needed to identify one case of colon cancer in asymptomatic, middle-aged persons.Here is a case report of the costs of colonoscopy… and why doctors almost always find a polyp to remove: they can bill more. Removing a polyp changes the procedure from “preventive to diagnostic.”
- Total Bill: $10,329 for the procedure, anesthesiologist, and gastroenterologist. Cigna’s negotiated rate was $4,144, and the patient’s share under her insurance was $2,185.
Doctors don’t know why these tiny nodules develop, but removing them is thought to ‘prevent cancer’ – even though only 5-10% of all polyps will become cancerous.
Effect of Colonoscopy Screening on Risks of Colorectal Cancer and Related Death
On October 9, 2022, The New England Journal of Medicine (NEJM) published a landmark study that dared to suggest colonoscopies are not as effective as previously thought. Colonoscopies were compared head-to-head against those who did not undergo cancer screening in a randomized trial that collected data over 10 years.
The large northern European trial that included nearly 85,000 people in a ten-year follow-up found an 18% reduction in colorectal cancer and a 50% reduction in risk of dying from colorectal cancer compared to an 88% death rate generally touted.Study researcher Dr. Michael Bretthauer, a gastroenterologist at the University of Oslo in Norway, said he found the results “disappointing” but worthy of consideration. He went on to say, “We may have oversold the message for the last 10 years or so, and we have to wind it back a little.”
Based on his results, screening colonoscopy reduced the risk of cancer by 18-31% and the risk of death from colon cancer by around 50%, much lower than generally promoted.
For decades, gastroenterologists have put colonoscopies on a pedestal, calling the procedure the “gold standard” for preventing colon cancer. In fact, clinicians believed that if everyone had this screening exam – a 66-inch rubber tube inserted in the rectum to view the colon – colorectal cancer would essentially become ‘extinct.’ But this new study (above), published in a peer-reviewed journal, brings to question colonoscopy’s dominance.
Routine Colonoscopies be Challenged
Colorectal screening is advocated for healthy, asymptomatic people; therefore, the risks from screening are important issues. As it turns out, more than 1,000 studies have reported serious complications after colonoscopy can occur.
Here’s an example:
A study published in 2006 in the Annals of Internal Medicine reviewed 35,945 charts of patients who had undergone colonoscopies within the Kaiser Permanente, Northern California (KPNC) health care system. This is what they found (whole numbers reported here for clarity):- Serious complications occurred in nearly 1 per 1000 exams without biopsy or polypectomy
- Serious complications other than bleeding occurred in 7 per 1000 exams with biopsy or polypectomy
- Bleeding occurred in nearly 5 per 1000 colonoscopies with biopsy62% of bleeding episodes and 40% of all serious complications occurred following removal of polyps smaller than 10 mm
- Perforation of the colon occurred more commonly with biopsy and occurred at a rate of almost 1 per 1000 exams
What does this study mean in real numbers?
Given that 15,000,000 colonoscopies are performed each year in the US alone, the study points out:
- Exam only, no biopsy/polypectomy: Up to 15,000 persons per year (1/1000) can have a serious complication – colon perforation, persistent pain/burning, persistent diarrhea, etc.
- Exam with biopsy/polypectomy: Up to 105,000 persons per year (7/1000) can have a serious complication
- 75,000 persons per year (5/1000) may experience extended bleeding that may result in hospitalization, surgery and/or need for blood transfusion.
- 15,000 persons per year (1/1000) may have a perforated colon. Small perforations are less likely to cause immediate peritoneal irritation and the diagnosis can be delayed for as long as 30 days, leading to poor prognosis.
A person can even die from a colonoscopy. The reported death rate after colonoscopy is around 0.09%. That sounds like a tiny number, but when applied to 15,000,000 exams per year, up to 13,500 person per year can die as a result of a colonoscopy!
The complication and death rate numbers have remained remarkably stable over the years. In fact, a 2016 meta-analysis evaluated post-colonoscopy complications by querying PubMed, Embase and the Cochrane library “for population-based studies” that had complications that started within 30 days of the exam. scomplications that were found within 30 days of the exam. The quiry found 1,074 studies published between January 1, 2001 and December 1, 2015. Even though, perplexingly, only 21 studies met the ‘inclusion criteria’ for their worldwide review, the results are very similar to those published in the 2006 study (discussed above).
Additional Complications
Most case reports are published to track serious complications, such as perforations or significant gastrointestinal bleeding occurring up to 4 weeks after the colonoscopy.
However, a 2010 study reviewed the risk of less serious complications. Researchers found that up to 33% of patients reported distressing gastrointestinal symptoms after the exam, including abdominal pain (10.5%), bloating (25%), self-limited gastrointestinal bleeding (3.8%), diarrhea (6.3%), and nausea (4.0%).
In a separate study, respiratory symptoms, including aspiration pneumonia, were found to rise approximately one week after colonoscopy. The study stated,
“As the rates of using deep sedation with anesthesia during colonoscopy have increased markedly in recent years, there is concern that respiratory complications may be an increasingly common event.”Risks of Infection after Colonoscopy
Remember that each year in the United States, more than 15 million colonoscopies and 7 million upper-GI endoscopies are performed on generally healthy individuals. Both procedures are performed with an endoscope, a reusable optical instrument that can be cleaned but not sterilized. In 2018, a study evaluated the rates of infection after colonoscopy and upper GI exams done in ambulatory surgery centers across the US. What was discovered was that the rates of infection was “far higher than previously believed, and varied widely from one ambulatory surgery center to another.”
This study was the first to explore data on ambulatory surgery centers (ASC) and post-procedure infection.Previously, post-endoscopic infection rates were thought to be around one event per million. The actual rate of infection within 7 days was found to be 1.1 per 1000 screening colonoscopy procedures; 1.6 per 1000 non-screening colonoscopy procedures (has a biopsy) and 3.0 per 1000 EDG procedures.
The rate of infections varied widely in different out-patient centers, ranged from 0 to 115 per 1000 procedures for screening colonoscopy; 0 to 132 for non-screening colonoscopy (polyp removed) and 0 to 62 for upper endoscopy.
Patients who’d been hospitalized before undergoing one of the procedures were at even greater risk of infection. Almost 45 in 1,000 patients who’d been hospitalized within 30 days prior to a screening colonoscopy returned to hospital or had an ER visit with an infection within a month. ‘
When these numbers are put in perspective of the total number of exams done per year (15,000,000), they are quite shocking:
- 0 to 115 infections per thousand colonoscopies ranges from 0 to 1,725,000
- 0 to 132 infections per thousand colonoscopies that remove a polyp ranges from 0 to 1,980,000
- 0 to 62 infections per thousand upper endoscopies ranges from 0 to 930,000
- If hospitalized within 30 days of one of these procedures, up to 675,000 person can have an adverse event
That puts things into a different perspective, doesn’t it?
Colon Perforation
Perforations of the colon result in a leakage of stool into the abdominal cavity resulting in peritonitis, sepsis, and/or septic shock. In a 2019 study, 741 cases of colon perforation caused by colonoscopy were reviewed. Surgical interventions were employed in 75% of the patients, of these 15% were laparoscopic and 85% required laparotomy (opening the abdomen – a major surgery).
Management of colon perforations from a colonoscopy depends on the location of the puncture or tear, the severity of the infection (local pain vs systemic sepsis), and the general overall health of the patient. Some patients may be treated with broad-spectrum antibiotics and abdominal physical examinations every 3–6 hrs. The close watch is to monitor for increasing pain and fever, which would require emergency surgical clean out and repair. The overall complications from the surgery (operative morbidity) has been reported to be 21–44% with a mortality rate of 7–25%. Those at highest risk of perforation include patients with a known, large lesion, unremitting colitis, or an obstructing lesion.
The Skill of the Examiner
A topic almost never discussed is how skilled is your doctor? Afterall, we are told to get a colonoscopy to remove polyps that ‘just might’ become cancer. We assume that all doctors are adequately trained and experts in their field.
In 2010, an analysis of all colonoscopies performed between 1995 and 2008 were reviewed and compared against the experience of the endoscopist. This included a review of more than 25,000 procedures. This important study concluded:
“The relative risk (RR) ratio was highest for endoscopists performing less than 591 procedures per year. Colonoscopy carried out by a low-volume endoscopist was independently associated with bleeding and perforation.”Colonoscopy is an invasive procedure, and a significant skill set is necessary to do it safely. A study from 2000 of colon perforations from reported,
“Although trainee endoscopists were involved in only 20% of the colonoscopies performed, eight (40%) perforations occurred while the training fellow was involved in the case.”Recall that the primary reason doctors advocate for colonoscopies is to remove polyps. Patients assume “they got it!” when they are told a polyp has been removed.
Not so fast.
While the benefits of colonoscopy have long been promoted, its accuracy is rarely questioned.
In 2008, a study to assess the rate of missed adenomas was undertaken using a strict methodology to limit related to the technique used or to the expertise of the operator. A pooled miss rate for the first procedure was calculated as the total number of lesions missed by the first procedure divided by the total number of lesions found. A total of 286 patients completed both exams.
Among the 165 patients believed to be free of polyps after the first examination, 67 (41%) were found to have at least one polyp on the second examination whereas among the 191 patients believed to be free of adenomas on first colonoscopy, 27 (14%) were found to have at least one adenoma on the second procedure.A similar study was done a few years later (2012) in Korea. Back-to-back colonoscopies by two different clinicians on the same day were performed on 149 patients. A total of 344 polyps (neoplastic and non-neoplastic polyps) were found, while 58 polyps (adenomatous and non-adenomatous) and 42 adenomatous polyps were missed, equating to a ‘miss rate’ of 17%. The overall rate of missed polyps, pooled from several studies, can range from 6 to 27%.
Although colonoscopy as a tool will never be perfect, safety is critical and should be questioned. It is important to know the TRUE, evidence-based risks for colonoscopy complications before consenting to this as a “screening” procedure.
For example: be sure to ask the physician doing the colonoscopy is, “How many of these procedures do you do per year?” and tell them, “I prefer to not have a resident (a doctor in training) do my test.”

.png)




.png)
.png)
.png)
Comments
Post a Comment