Linoleic Acid and Cancer Growth: What a 2025 Study Really Found
A New Mechanism Links Dietary Fat to Aggressive Breast Cancer — With Important Caveats
Researchers at Weill Cornell Medicine have identified a specific biological mechanism through which omega-6 linoleic acid — a fatty acid common in Western diets — may promote the growth of an aggressive form of breast cancer. The study, published in the journal Science, is being widely discussed online, but the findings are more precise — and more limited — than many headlines suggest.
Here is a clear-eyed breakdown of what the research found, what it means for different people, and what questions remain unanswered.
What Is Linoleic Acid?
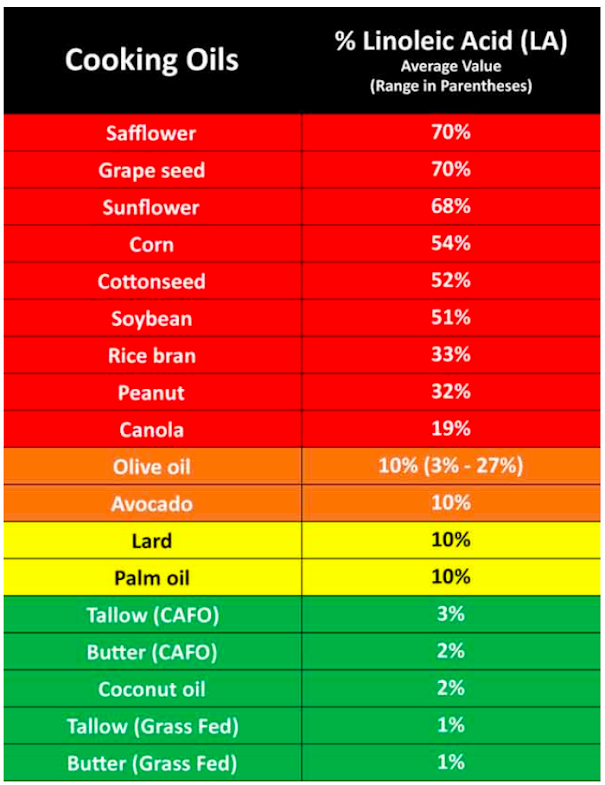
Linoleic acid (LA) is an omega-6 polyunsaturated fatty acid and an essential nutrient — meaning the human body cannot produce it on its own and must obtain it through food. It is found in:
- Vegetable and seed oils (sunflower, soybean, safflower, corn)
- Nuts and seeds
- Poultry and eggs
- Many packaged and processed foods
What the Study Found
The Weill Cornell study, published in Science (1), investigated how linoleic acid interacts with triple-negative breast cancer (TNBC) — one of the most aggressive and treatment-resistant forms of breast cancer, which lacks estrogen, progesterone, and HER2 receptors.
The Key Mechanism: FABP5 and mTORC1
The researchers discovered a two-step process:
- FABP5 acts as a transporter. Fatty acid binding protein 5 (FABP5) — a protein found at elevated levels in TNBC tumors — picks up linoleic acid and shuttles it into cancer cells.
- mTORC1 is activated. Once inside, linoleic acid triggers mTORC1 (mechanistic target of rapamycin complex 1), a well-known cellular growth switch that signals cells to divide and multiply.
In animal models, mice with TNBC that were fed a high-LA diet developed larger, faster-growing tumors compared to mice on a lower-LA diet. The effect was tied directly to FABP5 expression: tumors with higher FABP5 levels showed stronger responses to dietary LA.
"This discovery helps clarify the relationship between dietary fats and cancer, and sheds light on how to define which patients might benefit the most from specific nutritional recommendations in a personalized manner."
— John Blenis, PhD, Senior Author, Weill Cornell Medicine
Why This Research Matters
This study is scientifically significant for several reasons:
- It is the first to identify a specific molecular mechanism linking dietary omega-6 linoleic acid to cancer cell growth — previous research had produced mixed or inconclusive results.
- It points toward FABP5 as a potential biomarker — patients whose tumors express high FABP5 may one day receive personalized dietary or therapeutic recommendations.
- The mTORC1 pathway is already a major target in cancer drug research, so this connection opens additional avenues for treatment development.
Co-author Nikos Koundouros, PhD, noted there may be "a broader role for FABP5-mTORC1 signaling in other cancer types and even in common chronic diseases such as obesity and diabetes" — though this remains speculative and requires further study.
What the Study Does NOT Mean
This is where accurate reporting matters most. Several things this study does not show:
1. It does not prove LA causes cancer in humans
The research was conducted in animal models and cell cultures. Translating animal study results to human dietary recommendations requires large, long-term clinical trials — none of which yet exist for this specific mechanism.
2. It does not apply to all cancers — or all people
The FABP5-mTORC1 pathway was identified specifically in triple-negative breast cancer, which has unusually high FABP5 expression. Other cancer types — and healthy cells — respond very differently to linoleic acid. In fact, separate research has found LA exhibits anti-proliferative effects in endometrial cancer, and its effects in colorectal cancer appear dose-dependent.
3. Large population studies show no increased overall cancer risk from LA
Multiple large human cohort studies have found no significant association between typical dietary linoleic acid intake and increased overall cancer risk. Some studies have found inverse associations — meaning higher LA intake correlates with lower incidence of certain cancers.
4. Linoleic acid is an essential nutrient, not a toxin
The body requires LA for normal function. Recommending intake below 5 grams per day — far below typical needs — is not supported by current nutritional science and could create deficiencies affecting skin health, hormone production, and immune function.
What This Means for Diet and Cancer Prevention
Based on the totality of current evidence, here is what is reasonable to conclude:
For the general population:
There is no strong evidence that reducing linoleic acid below normal levels reduces cancer risk. Standard dietary guidance — eating a varied, whole-food diet, limiting ultra-processed foods, maintaining a healthy weight, and avoiding smoking — remains the best-supported approach to cancer risk reduction.
For TNBC patients and high-risk individuals:
This research suggests that FABP5 expression levels may one day inform personalized dietary guidance for TNBC patients. Oncologists and registered dietitians are the right source of advice here — not general population dietary rules.
What the evidence does support:
Reducing ultra-processed food consumption is associated with improved health outcomes across multiple disease categories. Many processed foods are high in LA and refined carbohydrates, added sugars, and sodium — all of which have independent health implications.
Frequently Asked Questions
Q: Should I stop eating seed oils because of this study?
A: No — not based on this study alone. The research identified a mechanism in a specific cancer type using animal models. Broad dietary changes for the general public are not supported by this evidence.
Q: Is linoleic acid bad for you?
A: At normal dietary levels, no. LA is an essential fatty acid. The concern in this study is about a specific mechanism in a specific cancer type (TNBC), particularly in people whose tumors express high levels of FABP5.
Q: What is FABP5 and should I get tested for it?
A: FABP5 is a protein found at elevated levels in some aggressive cancers, particularly TNBC. It is not currently a standard clinical test, but it may become a useful biomarker as this research develops.
Q: What dietary fats are safest?
A: Current evidence supports a diet rich in a variety of fats — including monounsaturated fats (olive oil, avocado), omega-3 fatty acids (fatty fish, flaxseed), and modest amounts of saturated and polyunsaturated fats. Extreme restriction of any single fat type is generally unnecessary for healthy individuals.
Q: Will reducing linoleic acid cure or prevent cancer?
A: No evidence currently supports this claim. If you have been diagnosed with cancer, work with your oncologist and a registered dietitian for evidence-based nutritional guidance.
The Bottom Line
The Weill Cornell Science study is a meaningful scientific contribution. It identifies, for the first time, a specific pathway through which dietary linoleic acid may accelerate triple-negative breast cancer growth in animal models — and points toward FABP5 as a potential therapeutic and dietary target for a subset of cancer patients.
What it does not do is justify sweeping dietary restrictions for healthy people, nor does it overturn decades of nutritional research establishing linoleic acid as an essential and generally beneficial nutrient.
As with most early-stage mechanistic research, the right response is continued investigation — not alarm. Future clinical trials examining FABP5 expression and dietary fat in TNBC patients will be the necessary next step before any firm recommendations can be made.
This article is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare provider before making changes to your diet or health regimen.
Sources:
- Koundouros N, et al. Science, 2025. DOI: 10.1126/science.adm9805
- Weill Cornell Medicine press release, April 1, 2025
- Qiu J, et al. Cancer Biology & Therapy, 2024. DOI: 10.1080/15384047.2024.2325130
- Johnson GH, Fritsche K. Journal of the Academy of Nutrition and Dietetics, 2012

.png)




.png)
.png)
.png)
Comments
Post a Comment